
Greater Queens Podiatry, PLLC
 (718) 229-0222
(718) 229-0222
 (718) 229-0222
(718) 229-0222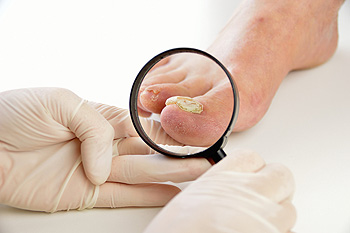 A common foot ailment that many patients suffer from is known as toenail fungus. The medical term for this contagious condition is referred to as “onychomycosis”. There are several noticeable symptoms that are associated with toenail fungus including thickening of the nail, discoloration, and cracking. Diabetic patients may be more susceptible, due to a weakened immune system. Additionally, if there has been an injury that has happened to the nail, or if circulation problems exist, these conditions may lead to the development of toenail fungus. Research has indicated that there are methods that can be implemented which may help to prevent this condition from occurring. These can include wearing appropriate shoes while in public swimming pools and surrounding areas, avoiding sharing nail clippers, and keeping the feet clean and dry. If you have this ailment, please consult with a podiatrist who can offer the proper treatment solutions.
A common foot ailment that many patients suffer from is known as toenail fungus. The medical term for this contagious condition is referred to as “onychomycosis”. There are several noticeable symptoms that are associated with toenail fungus including thickening of the nail, discoloration, and cracking. Diabetic patients may be more susceptible, due to a weakened immune system. Additionally, if there has been an injury that has happened to the nail, or if circulation problems exist, these conditions may lead to the development of toenail fungus. Research has indicated that there are methods that can be implemented which may help to prevent this condition from occurring. These can include wearing appropriate shoes while in public swimming pools and surrounding areas, avoiding sharing nail clippers, and keeping the feet clean and dry. If you have this ailment, please consult with a podiatrist who can offer the proper treatment solutions.
For more information about treatment, contact our podiatrists of Greater Queens Podiatry, PLLC. Our doctors can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our office located in Bayside, NY. We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Read more about How to Treat Your Toenail FungusWhile not a serious issue, toenail fungus, or onychomycosis, can be an embarrassing and uncomfortable condition to experience. Toenail fungus is often caused from public areas that harbor fungi and improper cleaning/drying of the foot. Once infected, the fungus grows deeper into the nail and can be very hard to get rid of.
There are different types of fungus that cause toenail fungus. Dermatophytes, yeasts, and molds are the most frequent forms of fungus to infect the toenail. Dermatophytes are the most common among the three. Symptoms associated with fungal nails include the discoloration of the toenail, brittleness, and in some circumstances, a smell. Pain is rarely a symptom caused by toenail fungus.
Diagnosis of fungal nails is generally a rather quick process. However podiatrists will make sure that the cause is not another condition such as lichen planus, psoriasis, onychogryphosis, or nail damage. Podiatrists will make use of fungal cultures and microscopy to verify that it is fungus.
While over-the-counter ointments are readily available, most are ineffective. This is due to the fact that the nail is very protective and that the fungus slips in between the nail plate and bed. Podiatrists can offer oral medication which currently provides the best results.
Ultimately, prevention is the best line of defense against toenail fungus. Avoid unsanitary public showers. If you do use a public shower, use shower shoes to provide your foot with protection. Once you are finished showering, make sure to thoroughly dry your feet. Fungi thrive in warm, dark, and moist places like sweaty, warm feet that are left dark in shoes all day.
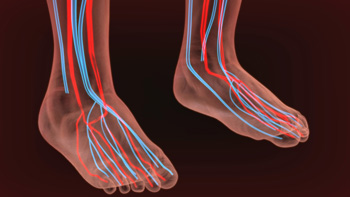 Peripheral artery disease, or PAD, is commonly caused by a buildup of plaque deposited in the walls of blood vessels. This plaque is made of cholesterol and fatty substances that can cause the arteries to become stiff and narrowed. Patients at the highest risk for developing PAD are those with diabetes or those who have a history of smoking. Other risk factors include high cholesterol, kidney disease and high blood pressure. Some symptoms that can occur from PAD are muscle cramps, reduced blood flow, weakness in legs and feet, color changes in the skin and dark purple or black spots that can develop on the toes. There are some ways to combat the symptoms. Standing and resting for a few minutes will cause the symptoms that stopped someone from walking to resolve. Also over time, people with PAD will tend to limit what they do in order to avoid symptoms, walk slower and use a cane. If you are currently experiencing symptoms of peripheral artery disease, it is advised that you schedule an appointment with a podiatrist.
Peripheral artery disease, or PAD, is commonly caused by a buildup of plaque deposited in the walls of blood vessels. This plaque is made of cholesterol and fatty substances that can cause the arteries to become stiff and narrowed. Patients at the highest risk for developing PAD are those with diabetes or those who have a history of smoking. Other risk factors include high cholesterol, kidney disease and high blood pressure. Some symptoms that can occur from PAD are muscle cramps, reduced blood flow, weakness in legs and feet, color changes in the skin and dark purple or black spots that can develop on the toes. There are some ways to combat the symptoms. Standing and resting for a few minutes will cause the symptoms that stopped someone from walking to resolve. Also over time, people with PAD will tend to limit what they do in order to avoid symptoms, walk slower and use a cane. If you are currently experiencing symptoms of peripheral artery disease, it is advised that you schedule an appointment with a podiatrist.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with our podiatrists from Greater Queens Podiatry, PLLC. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact our office located in Bayside, NY. We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Peripheral Artery DiseasePeripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.
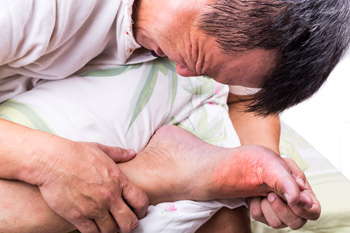 Gout is a painful condition that typically affects the joints of the big toe. It occurs as a result of excess uric acid in the bloodstream, which can cause crystals to form in the joints. Gout is a form of arthritis, and the symptoms that are most associated with this ailment often include swelling and redness surrounding the affected joints, severe pain and discomfort, and the area may feel warm. There are specific foods that have elevated purine levels, and this is a contributing factor to the onset of gout. These consist of red meat, alcohol, and certain types of seafood. It is beneficial to have a proper diagnosis performed, and this is often accomplished by extracting a portion of fluid that contains the crystals. Incorporating healthy lifestyle changes may be helpful in preventing future gout attacks. If you have this painful condition, it is advised that you consult with a podiatrist who can properly treat this ailment.
Gout is a painful condition that typically affects the joints of the big toe. It occurs as a result of excess uric acid in the bloodstream, which can cause crystals to form in the joints. Gout is a form of arthritis, and the symptoms that are most associated with this ailment often include swelling and redness surrounding the affected joints, severe pain and discomfort, and the area may feel warm. There are specific foods that have elevated purine levels, and this is a contributing factor to the onset of gout. These consist of red meat, alcohol, and certain types of seafood. It is beneficial to have a proper diagnosis performed, and this is often accomplished by extracting a portion of fluid that contains the crystals. Incorporating healthy lifestyle changes may be helpful in preventing future gout attacks. If you have this painful condition, it is advised that you consult with a podiatrist who can properly treat this ailment.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact our podiatrists from Greater Queens Podiatry, PLLC. Our doctors will treat your foot and ankle needs.
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions please feel free to contact our office located in Bayside, NY. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Everything You Need to Know About GoutGout, typically found in diabetic patients, is an unusually painful form of arthritis caused by elevated levels of uric acid in the bloodstream. The condition typically strikes the big joint on the big toe. It has also been known to strike the knees, elbows, fingers, ankles and wrists—generally anywhere that has a functioning, moving joint.
The high level of uric acid in a person’s bloodstream creates the condition known as hyperuricema—the main cause of gout. Genetic predisposition occurs in nine out of ten sufferers. The children of parents who suffer gout will have a two in ten chance of developing the condition as well.
This form of arthritis, being particularly painful, is the leftover uric acid crystallizing in the blood stream. The crystallized uric acid then travels to the space between joints where they rub, causing friction when the patient moves. Symptoms include: pain, redness, swelling, and inflammation. Additional side effects may include fatigue and fever, although reports of these effects are very rare. Some patients have reported that pain may intensify when the temperature drops, such as when you sleep.
Most cases of gout are easily diagnosed by a podiatrist’s assessment of the various symptoms. Defined tests can also be performed. A blood test to detect elevated levels of uric acid is often used as well as an x-ray to diagnose visible and chronic gout.
Treatment for gout simply means eliminating symptoms. Non-steroid anti-inflammatory drugs or NSAIDs (Colchicine and other corticosteroid drugs, etc.) will quell the redness, the swelling, and the inflammation. However, managing your diet, lifestyle changes, and using preventative drugs are all helpful toward fully combating the most severe cases.
Those that lead an inactive lifestyle are at a higher risk for gout. Any amount of exercise decreases the probability of repeat encounters with the condition. Reducing your consumption of red meat, sea food, and fructose-sweetened drinks also reduces the likelihood of chronic gout as well.
Ingesting Vitamin C, coffee, and particular dairy products can help with maintaining a healthy lifestyle. There are new drugs out on the market that inhibit the body’s production of uric acid-producing enzymes. However, reducing or eliminating your overall levels of uric acid is the best remedy to ensuring you lead a gout-free life.
Heel pain is a rather comm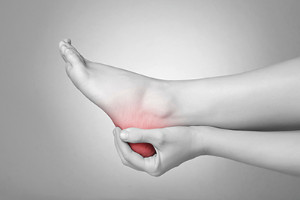 on foot problem. The pain will usually occur under the heel, towards the front of the heel, or just behind it, where the Achilles tendon connects to the heel bone. The most common cause of heel pain is plantar fasciitis, which is pain under the heel. Other causes include arthritis, heel bursitis and bumps, tarsal tunnel syndrome, stress fractures, Sever’s disease and Achilles tendinitis. The most common remedies for heel pain are rest, proper fitting footwear and applying ice to the afflicted area. If you are experiencing some kind of heel pain, it is suggested to go see a podiatrist.
on foot problem. The pain will usually occur under the heel, towards the front of the heel, or just behind it, where the Achilles tendon connects to the heel bone. The most common cause of heel pain is plantar fasciitis, which is pain under the heel. Other causes include arthritis, heel bursitis and bumps, tarsal tunnel syndrome, stress fractures, Sever’s disease and Achilles tendinitis. The most common remedies for heel pain are rest, proper fitting footwear and applying ice to the afflicted area. If you are experiencing some kind of heel pain, it is suggested to go see a podiatrist.
Many people suffer from bouts of heel pain. For more information, contact our podiatrists of Greater Queens Podiatry, PLLC. Our doctors can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Bayside, NY. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Heel PainHeel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
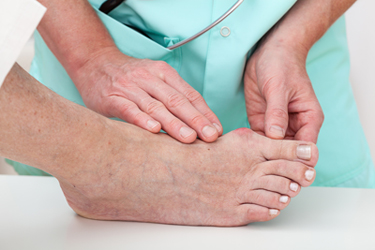 A bunion is described as a bony protrusion on the side of the big toe. It can develop as a result of genetic factors, or wearing shoes that do not have adequate room for the toes to move freely in. It is considered to be a bone deformity, and patients who have severe bunions may choose surgery as an option for permanent removal. The symptoms that are often associated with this condition can include pain in the joints of the big toe, calluses that form on top of the toe, and a shifting of the big toe toward the other toes. It may be difficult to wear shoes, in addition to having pain while walking or running. There are measures that can be implemented which may prevent bunions from developing. These include wearing shoes that fit properly, performing gentle foot stretches, or wearing shoe inserts that have adequate arch support. If you have developed a bunion, it is suggested that you speak with a podiatrist who can properly treat this condition.
A bunion is described as a bony protrusion on the side of the big toe. It can develop as a result of genetic factors, or wearing shoes that do not have adequate room for the toes to move freely in. It is considered to be a bone deformity, and patients who have severe bunions may choose surgery as an option for permanent removal. The symptoms that are often associated with this condition can include pain in the joints of the big toe, calluses that form on top of the toe, and a shifting of the big toe toward the other toes. It may be difficult to wear shoes, in addition to having pain while walking or running. There are measures that can be implemented which may prevent bunions from developing. These include wearing shoes that fit properly, performing gentle foot stretches, or wearing shoe inserts that have adequate arch support. If you have developed a bunion, it is suggested that you speak with a podiatrist who can properly treat this condition.
If you are suffering from bunion pain, contact our podiatrists of Greater Queens Podiatry, PLLC. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
Symptoms
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our office located in Bayside, NY. We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about BunionsA bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.
| Bayside Office 4401 Francis Lewis Blvd Suite L3B Bayside, NY 11361 Phone: (718) 229-0222 Fax: (718) 717-0275 | Monday: 9:30am - 7pm |
E-mail us with any questions